
When Robert Merton (1910 – 2003) dissected the allegory that we all are “standing on the shoulders of giants” — based on a much older saying by Bernhard of Chartres, according to John of Salisbury in 1159, often falsely attributed to Isaac Newton (1643-1727) who popularized it — (On the shoulders of Giants, published 1965), what he meant was that much of what we (scientists) are taking for granted and as starting points for new explorations, discoveries, and interventions are based on the pathways others have paved before us, and without them, our insights (or far-sights) would be much less. These “giants” are often well ahead of their time.
Much has been written about the historical origins of the use of placebos in medicine, e.g. (1), some of which will be subject of a future posting; beyond use of placebos in individual patients by individual doctors, the first placebo-controlled trials occurred in the first half of the last century in different subspecialties in medicine, e.g. in psychiatry (2).
But when you look at the distribution of genuine placebo publications in our database (3) (Figure) it was not before the late 1950ies when placebo research started to slowly grow, and two milestone papers mark the beginning of it: Henry Beecher’s ever-since-cited paper, “The Powerful Placebo,” of 1955 (4), and Stewart Wolf’s almost completely forgotten, “The Pharmacology of Placebos,” of 1959 (5). The different fates of these two giants of placebo research and their classic papers will be the topic of this and the next posting.
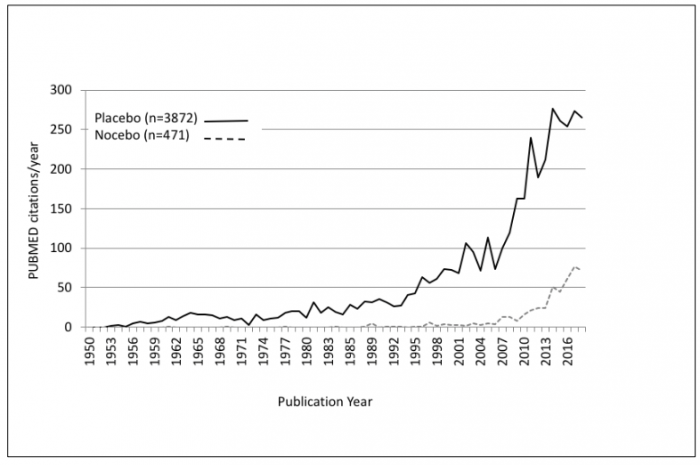
Figure: Number of genuine placebo and nocebo research papers in our database (3) (Note that placebo papers include papers on nocebo as well).
The two sides of Beecher’s work
Henry K. Beecher (1904 – 1976) was a Boston-trained and based anesthesiologist at Harvard Medical School who served as US Army surgeons in Africa and Italy during World War II. During these years (1939 to 1945), he published a number of articles relating to his battlefield medical experiences, related to pain and sedation, anesthesia, and analgesia in wounded soldiers, e.g. (6).
One of the most cited stories in public media, however, seems related to casual reports rather than systematic evaluation, namely that under shortage of opioids for pain management, injections of saline with confirmation that it was a drug would relieve the pain of soldiers as well — indication of a strong placebo response. We have not been able to identify any published source for this story and assume that Beecher may have told this during one or more of his presentations; battlegrounds are no solid basis for research, let alone placebo research.
Back in Boston after the war, Beecher published — among others — studies on pain control with analgesics (morphine, codeine, ASA) and was among the first to claim that placebo controls are necessary to estimate the efficacy of analgesics in pain control, as the placebo effect can account for up to 50% of the clinical efficacy of drugs, depending both on the analgesic and on the patient. Beecher noted placebo “reactors” and “non-reactors” and but avoids to speculate about their characteristics — until today, placebo responders and their personality are a quest to science.
His break-through as the “godfather” of placebo research, as which he is seen by some nowadays, came with his 1955 paper, “The Powerful Placebo,” (4) in which he summarizes in a kind of “meta-analysis” of previously-published research on the placebo effects of placebo-controlled interventions in pain and other conditions, e.g. nausea, cough, cold, anxiety. This meta-analysis does not — of course — withhold current standards of meta-analyses, but nonetheless raised substantial discussion, both pros and cons, to his position. He estimated the placebo effect in clinical trials to be on average 35%, which comes close to similar numbers when more appropriate statistics and more homogeneous conditions and interventions are used, e.g. (7).
Opponents (8) have argued that this overestimation is due to the fact that most — if not all — studies have not controlled for spontaneous variation and symptom relief, and respective analyses, in fact, show that about 50% of the placebo response in RCT is accountable to such methodological errors and biases (9). Whether this then makes the placebo powerless, as has been argued, remains to be shown, not in meta-analyses but in clinical trials and practice.
Henry K Beecher’s “dark side” is his obscure involvement in secret service (CIA) interrogations of prisoners-of-war during and after the war using drugs such as mescaline, which has been documented much later, after the turn of the century (10). Beecher has also reviewed reports from and reported to the CIA and met with Nazi physicians that had conducted inhumane experiments with prisoners of concentration camps, such as Walter Schreiber during his CIA imprisonment and interrogation.
Interestingly, homage papers for Henry K. Beecher such as (11) do not even mention this controversy at all; instead, they emphasize that, in the late 50s, Beecher was the promoter of medical ethics and the ethical conduct of medical research not only at Harvard Medical School but in the US and abroad (12) — maybe an attempt for absolution for this ethically questionable involvement (13).
What remains, what is dismissed
Even critics of Beecher’s position of a “powerful placebo” cannot ignore that the integration of a placebo arm in randomized controlled trials (RCTs) and the assessments of the true drug effects as the difference between drug and placebo arm response represents a major achievement. And it is generally accepted that this difference represents a compound of spontaneous variation/remission, assessment biases (regression to the mean), and expectancy and conditioning effects of the psychosocial setting that constitutes the medical environment of every treatment. Even psychotherapy underlies these rules, as we have shown.
Questioning the relative contribution of each of these factors to the overall placebo effect ignores the variable contributions of the disease and its characteristics, the role of patient characteristics, and the constituents of the doctor-patient relationship and communication throws the baby out with the bathwater. What remains is tedious science and eventually contradictions between clinical trials, meta-analyses of RCT, and experimental work on the same topic, the placebo effects.
A major concern of Beecher’s critics is the lack of control for spontaneous variation of symptoms in all RCT, before any conclusion about the size of the placebo effect can be drawn. Here, novel study designs are needed, which control not only for drug versus placebo differences, but also allow for a comparison to conventional treatment (“real life” studies) as well as to non-treatment controls, such as the Cohort Multiple Randomized Controlled Trial (CMRCT) (14) — this will be discussed another time.
What also remains is the need for thorough ethics in placebo research. Providing a placebo to a patient in need (and in search) of therapy is already an ethical challenge that the World Medical Association (WMA) has set limits on with the Declaration of Helsinki (15). Experimental placebo research, when conducted in healthy volunteers, faces another quest: Similar to lie research (How to identify a person lying? What strategies do liars use to hide their behavior? etc., of interest to interrogators, lawyers, and law enforcers), placebo research frequently uses deception as a tool to provoke placebo responses, e.g. the promise to apply a powerful drug when instead a placebo is given following an experimental pain stimulus. This has caused concerns among ethicists (16), requesting fully-informed consent for trial participation and alternatives such as authorized deception (17) and open-label placebo which have been developed and that we will discuss another time.
Giants standing on my shoulders
Merton’s pleasant reading “On the Shoulders of Giants,” (1965) lists 46 variants of interpretation of this popular allegory throughout the centuries, many of which mirror scientists timidly claiming either to be the giant or hypocritically being the dwarf that sees farther anyway. A contemporary and unique quote attributed to MIT professor Hal Albertson would have found Merton’s approval: “If I have not seen as far as others, it is because giants were standing on my shoulders.”
Sometimes, it appears that giants must step aside to allow for a different view — and maybe a paradigm shift — on the topic they occupy. Placebo research in the aftermath of Beecher’s “powerful placebo” statement may be such an occasion: while it has helped the term placebo to receive attention in the medical community in the past, it may hinder the future development of placebo research if his view is taken forward forever.
This is part 11 of a series covering “placebo” provided by Paul Enck and Sibylle Klosterhalfen from the Tübingen University Hospital. Continuous updates on placebo research can be found at www.jips.online.
References:
- Jutte R. The early history of the placebo. Complementary therapies in medicine. 2013;21(2):94-7.
- Shorter E. A brief history of placebos and clinical trials in psychiatry. Canadian Journal of psychiatry/Revue canadienne de psychiatrie. 2011;56(4):193-7.
- Enck P, Horing B, Broelz E, Weimer K. Knowledge Gaps in Placebo Research: With Special Reference to Neurobiology. International review of neurobiology. 2018;139:85-106.
- Beecher HK. The powerful placebo. Journal of the American Medical Association. 1955;159(17):1602-6.
- Wolf S. The pharmacology of placebos. Pharmacological reviews. 1959;11:689-704.
- Beecher HK. Anesthesia for Men Wounded in Battle. Annals of surgery. 1945;122(5):807-19.
- Papakostas GI, Fava M. Does the probability of receiving placebo influence clinical trial outcome? A meta-regression of double-blind, randomized clinical trials in MDD. European neuropsychopharmacology. 2009;19(1):34-40.
- Hrobjartsson A, Gotzsche PC. Is the placebo powerless? Update of a systematic review with 52 new randomized trials comparing placebo with no treatment. Journal of internal medicine. 2004;256(2):91-100.
- Krogsboll LT, Hrobjartsson A, Gotzsche PC. Spontaneous improvement in randomised clinical trials: meta-analysis of three-armed trials comparing no treatment, placebo and active intervention. BMC medical research methodology. 2009;9:1.
- McCoy AW. Science in Dachau’s shadow: Hebb, Beecher, and the development of CIA psychological torture and modern medical ethics. J Hist Behav Sci. 2007;43(4):401-17.
- Miller FG. Homage to Henry Beecher (1904-1976). Perspectives in biology and medicine. 2012;55(2):218-29.
- Miller FG. Henry Beecher and Consent to Research: a critical re-examination. Perspectives in biology and medicine. 2016;59(1):78-94.
- Mashour GA. Altered states: LSD and the Anesthesia Laboratory of Henry Knowles Beecher. Bulletin of anesthesia history. 2005;23(3):11-4.
- Relton C, Torgerson D, O’Cathain A, Nicholl J. Rethinking pragmatic randomised controlled trials: introducing the “cohort multiple randomised controlled trial” design. Bmj. 2010;340:c1066.
- Skierka AS, Michels KB. Ethical principles and placebo-controlled trials – interpretation and implementation of the Declaration of Helsinki’s placebo paragraph in medical research. BMC medical ethics. 2018;19(1):24.
- Miller FG, Wendler D, Swartzman LC. Deception in research on the placebo effect. PLoS medicine. 2005;2(9):e262.
- Martin AL, Katz J. Inclusion of authorized deception in the informed consent process does not affect the magnitude of the placebo effect for experimentally induced pain. Pain. 2010;149(2):208-15.









