
Everyone knows someone who has had their tonsils taken out at some point in their lives. In some families, it is practically a rite of passage, as once children reach a certain age, they are inevitably taken to the doctor for various complaints, mostly related to noisy breathing, mucous or salivary excess, or frequent “throat infections.” They will typically undergo some testing, and, once complete, these children are typically scheduled for removal of the tonsils and usually its nasal companion known as the adenoids.
This practice, along with many other variations on airway surgery in adults and children has been booming throughout the 20th and 21st centuries, conducted mostly by specialists known as Otolaryngologists, commonly called ear, nose, and throat surgeons. For the most part, the practice has been questioned by few, but a recent article from a team of non-clinician researchers from Denmark reviewed the records of over a million children and unexpectedly found that the children who had their tonsils and adenoids removed had a two- to three-fold increase in a variety of respiratory diseases as the primary differentiating factor from the general population. In other words, in the long run, these children may be experiencing a higher rate of the problem than the procedures were attempting to prevent.
While this finding may be shocking to some, it probably is not to a Stanford sleep specialist named Christian Guilleminault. Guilleminault has spent a lifetime studying how facial and dental structure relate to the airway, the tonsils, and sleep disorders, publishing over 700 papers. But, unlike some of the surgical researchers that tend to focus on examining variations in technique, Guilleminault has been questioning the whole treatment paradigm, and instead has proposed an entirely different pathway.
Most active clinicians utilize a specific cascade of cause and effect events when describing the childhood (and adult) sleep disorders to their patients. In summary, the conventional model proposes that a vague infectious (like strep throat) or inflammatory (allergy) event in the child’s throat is the initial inciting event, which causes growth of excess immune cells in the child’s tonsils and adenoids. Then, these structures continue to grow, causing blockage during sleep creating snoring, also causing excess production of mucous and salivary discharge, and further pre-dispose toward throat infection. Clinicians and parents usually agree that the best course of action is the removal of these offending agents. Further, most clinicians, informed by limited but widely-publicized animal experiments from the 1980s, caution parents that failure to remove the tonsils and adenoids could result in a facial deformity known as “adenoid face,” a long face with a recessive chin.
In contrast, our article reviews the alternative chain of events, mostly proposed by Guilleminault and his research colleagues. In this reverse-order paradigm we call Guilleminault’s Musculoskeletal Hypothesis (GMH), essentially the exact opposite of the conventional cause-and-effect is suggested. Using this pathway, our paper provides the anatomic mechanisms to explain how this actually may work and to suggest to clinicians potential solutions.
In this alternate view, the initial problem lies with limitations in growth of the facial skeleton and muscular tone. This is not to suggest that the growth problems are severe, pathologic, or part of a disease, but just subtle restriction in facial growth within the normal spectrum of appearance that predisposes individuals to airway disorders. Over the course of human evolution, the skeletal structures of the cheeks and jaw have been progressively becoming more set-back from their original snout-like positions. It is not clear why this has occurred, but many scientists have considered that changes in diet, activity level, and even considerations of attractiveness may have played a role in making these bony structures less robust. The progressive nature of the receding facial bones over millennia may have resulted in an increase in this rate over the last century of industrialization.
Variations in the shape of the jaw bone (see figure) with downward rotation of the tooth-bearing segment may predispose people to mouth-breathing instead of the preferred nasal breathing route. Further, this subtle change in structure of the lower jaw causes alteration of the upper jaw or maxilla, which influences the nose to sustain bony crowding. This bony crowding can create a situation where the middle wall between the nostrils, or the septum, becomes warped and bulges at the bridge of the nose, creating a classic “bump.” This subtle skeletal change causes an open-mouthed appearance, a subtle nasal deformity, reduced nasal airflow, and a stronger tendency to night-time mouth- breathing.
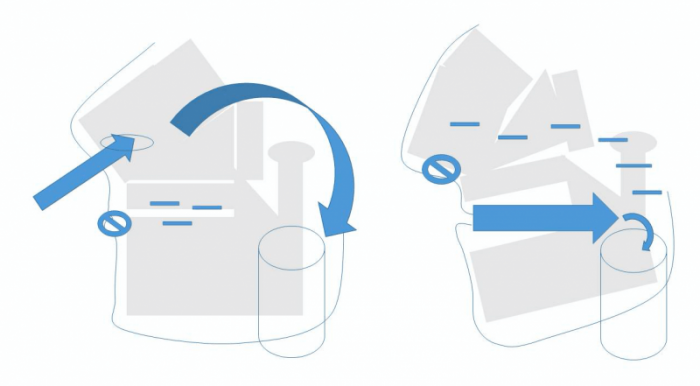
Figure Caption: Left: Model of Facial Structure Predisposed to Primarily Nasal Breathing. Right: Model of Facial Structure Predisposed to Primarily Mouth Breathing. Key: Blue arrows – airflow direction, Cylinder – Throat or Pharynx, “Not” sign – closed air passage, Minus sign – negative pressure indicator. Image courtesy Howard D. Stupak
While seemingly innocuous, mouth-breathing at night causes a host of problems from causing more infections due to dryness of the throat passages (Guilleminault 2018) to chronic sleep disorders. The sleep disorders due to mouth breathing are due to a buildup of vacuum pressure in the nose and parts of the throat (or pharynx) due to an under-utilized nasal passage. Also, the tongue itself during sleep-time nasal breathing is locked in position between the upper and lower jaws. During sleep-time mouth-breathing, the tongue, a large muscle, can fall backwards into the throat, thus constricting the airway. This vacuum force, combined with tongue collapse and exacerbated by gravitational forces, results in an environment in the throat that predisposes to restricted airflow noises (snoring) and poor respiration (sleep apnea).
This dry, vacuum-like environment may damage the throat tissues, actually drawing the wall tissue into the air passage, and potentially triggering the actual growth of the tonsils and adenoids themselves, although these late-comers were long believed to be the sole culprits of disease!
Thus, the exact order of the problem is perfectly reversed, where the facial structure anomaly is the initial event, causing mouth-breathing which subsequently causes a sleep-breathing disorder. The chronic nature of this disorder may predispose the throat to dryness, mucous discharge, and growth of the tonsils and adenoids.
What are the implications of this? Many. If the initial problem is facial structure and mouth-breathing, then removing the tonsils and adenoids will not address the primary problem, despite what is commonly believed. Interestingly, synthesizing the scientific literature shows that success rates for adenoid-tonsillectomy approach only 50%, while a Cochrane database analysis shows a similar success rate for non-surgical observation. What if the 50% of patients that achieved success were the same patients that would have succeeded with observation only, while the 50% that failed only failed because of their facial structure, and mouth-breathing was not amenable to waiting for facial growth?
what should be done instead of (or at least in addition to) surgery for these patients? Or, more appropriately, what did I do for my own son who had these problems? A combination of mouth-closure techniques using appliances or garments, and a strategy to encourage jaw growth using dental devices or surgery. Of course, we continue to require more evidence to further support this alternative pathway.
These findings are described in the article entitled Gravitational forces, negative pressure and facial structure in the genesis of airway dysfunction during sleep: a review of the paradigm, recently published in the journal Sleep Medicine. This work was conducted by Howard D. Stupak and Steven Y. Park from the Albert Einstein College of Medicine.
References:
- Byars SG, Stearns SC, Boomsma JJ. Association of Long-Term Risk of
Respiratory, Allergic, and Infectious Diseases With Removal of Adenoids and
Tonsils in Childhood. JAMA Otolaryngol Head Neck Surg. 2018 Jul 1;144(7):594-603. - Stupak HD, Park SY. Gravitational forces, negative pressure and facial structure in the genesis of airway dysfunction during sleep: a review of the paradigm. Sleep Med. 2018 Nov;51:125-132.
- Lee SY Guilleminault C, Chiu HY, Sullivan SS. Mouthbreathing, “nasal disuse” and pediatric sleep-disordered breathing.Sleep Breath (2015) 19: 1257-64
- Kukwa W, Guilleminault C, Tomaszewska M, Kukwa A, Krzeski A, Migacz E. Prevalence of upper respiratory tract infections in habitually snoring and mouth breathing children. Int J Pediatr Otorhinolaryngol. 2018 Apr;107:37-41.
- Tomer BS, Harvold HP. Primate experiments on mandibular growth direction. Am J Orthod. 1982 Aug;82(2):114-9.
- Venekamp RP1, Hearne BJ, Chandrasekharan D, Blackshaw H, Lim J, Schilder AG Tonsillectomy or adenotonsillectomy versus non-surgical management for obstructive sleep-disordered breathing in children. Cochrane Database Syst Rev. 2015 Oct 14;(10):CD011165.
- Sleep. 2014 Jan 1;37(1):71-6. doi: 10.5665/sleep.3310. Treatment outcomes of adenotonsillectomy for children with obstructive sleep apnea: a prospective longitudinal study. Huang YS(1), Guilleminault C(2), Lee LA(3), Lin CH(4), Hwang FM(5)
- Weinstock MS, Stupak HD. Bony/Cartilaginous Mismatch: A Radiologic
Investigation into the Cause of Tension Nose Deformity. Plast Reconstr Surg. 2018
Feb;141(2):312-321. - Zang HR, Li LF, Zhou B, Li YC, Wang T, Han DM. Pharyngeal aerodynamic characteristics of obstructive sleep apnea/hypopnea syndrome patients. Chin Med J (Engl). 2012 Sep;125(17):3039-43.









