
In recent years, immunization rates for children in the United States have been steadily declining in conjunction with an increase in reported outbreaks of infectious diseases. In general, evidence suggests that vaccine rates decline as children age: they are highest among infants and children entering school, but lower for adolescents, and there is considerable variation across states. State and local law generally mandates childhood vaccines prior to enrollment in school and at regular intervals thereafter, but the use of non-medical vaccine exemptions has been steadily on the rise, reflecting increased vaccine hesitancy (Omer et al. 2009).
While there is evidence that state laws on exemption procedures influence exemption rates (Wang et al. 2014; Richwine et al. 2019), relatively little is known about how best to administer these immunization requirements and communicate them to stakeholders in the school system. Evidence suggests that nudges can be a successful mechanism to alter physician behavior around adult vaccinations (Kiefe et al. 2001). However, nudges have not been utilized to target immunization behavior in a school-based setting.
A recent randomized controlled trial conducted by the Office of Evaluation Sciences in the U.S. General Services Administration analyzed targeted communications that utilized descriptive social norms with the objective of increasing immunization compliance in educational institutions (schools and day care centers) in a mid-size city. The sample included 700 schools and day care centers; they were randomly assigned to a treatment group that received a biannual immunization “report card,” or a control group.
The report card provided information about the school’s immunization compliance rates relative to other schools of the same type (daycare, elementary, middle, or high): more specifically, it highlighted average compliance, average compliance among top performers (the top 10%), and the school’s star rating. (Immunization compliance is defined in this jurisdiction as the percentage of students reporting completion of all required vaccines or the submission of an appropriate medical or non-medical exemption.) The report card was addressed to the school leader and also provided some information about action steps to increase compliance.
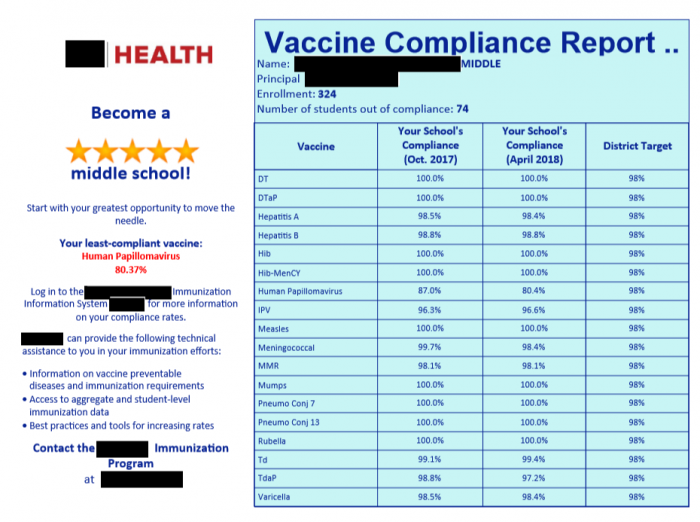

Images courtesy Jessica Leight
Data about school-level immunization compliance is available in a comprehensive immunization registry, and this data was used to evaluate the effects of the intervention by comparing compliance rates between the treatment and control group. The analysis suggests that the intervention did not shift compliance rates; the coefficient of interest is a precisely estimated null that allows us to rule out an increase in compliance larger than 2.8 percentage points, relative to a mean of 76%.
The absence of any significant effect of the report card is consistent with several potential hypotheses. The report card may not suffice to alter school leaders’ behavior in the absence of a clear incentive. Alternatively, school leaders may not have appropriate tools to affect parents’ immunization choices, or may simply not view school immunization policy as an important part of their responsibilities.
This RCT is the first evaluation to examine the use of descriptive social norms in altering school-based immunization rates. The evidence is consistent with recent literature that suggests that the increase in vaccine hesitancy is not easily targeted by traditional communications strategies and that new community-level tools may be needed (McClure et al. 2017).









