The field of biology is intimately connected to mechanics. In other words, life requires motion. And where there is motion, there is usually friction.
Friction, or the resistance of one surface to move over another, can sometimes be a beneficial phenomenon; it allows our cars to grip the road, our fingers to grip objects, and our sneakers to grip the floor when we change directions. In these cases, the presence of a lubricant, or an agent that reduces friction, can be detrimental; if you’ve ever hydroplaned while driving or lost your footing on slippery flooring, you can attest to the value to having friction.
But in many other situations, friction can lead to problems when there is too much of it. If materials need to slide over one another, and if the friction forces are too high, then they could cause mild nuisances such as sticking together (e.g. a delicate sunny-side-up egg that won’t slide off the frying pan) or making a squeaking sound (e.g. that pesky door hinge). Or they could cause more serious problems, such as heating to dangerous temperatures (e.g. industrial saws or a car’s engine) or getting severely damaged or even breaking (e.g. bearings and sliding elements in spacecraft).
These examples are classic mechanical problems. Your frying pan probably has a Teflon or a surface-modifying ceramic coating to allow the egg to slide right off, and you can spray WD-40 on the squeaky door hinge. High-speed saws and your car’s engine are lubricated by high-quality oils or other fluids, and spacecraft bearings and other high-performance mechanical components have special lubricant additives depending on the situation. In the latter example, the objective of using lubricants is to prevent wear (and ultimately failure); the study of wear, along with friction and lubrication, is known as tribology.
When it comes to tribological phenomena in biology, or biotribology, maintaining low friction is often imperative. We take about 2 million steps each year, which is only possible because our knee joints have an excellent lubricating fluid — synovial fluid — in them. We blink about 10 million times each year, thanks to the friction-lowering abilities of the tear film that our tear ducts produce. Food slides down our esophagus without getting stuck, and likewise exits the body as waste, because it gets coated with mucosal secretions in the mouth (saliva) and bowel. These various lubricants for biological interfaces, or biolubricants, work perfectly fine when the body is in a healthy state.
But again, just like in the mechanical world, the biological world can have problems of high friction. These diseases include osteoarthritis (decreased concentrations of lubricating macromolecules in synovial fluid), dry eye (decreased viscosity of tear film), dry mouth (decreased secretion of saliva), and others, including vaginal dryness, intraabdominal adhesions after surgery, and dry skin (lotion, and even Chap Stick, can be considered lubricants).
To improve the body’s own biolubrication processes, there are three main categories of biotribological therapeutics: drugs, biomaterials, and physical techniques. In our recent review article, we provide an overview of the landscape of these treatments addressing challenges in biotribology, along with the future directions of these subfields due to emerging technologies under development.
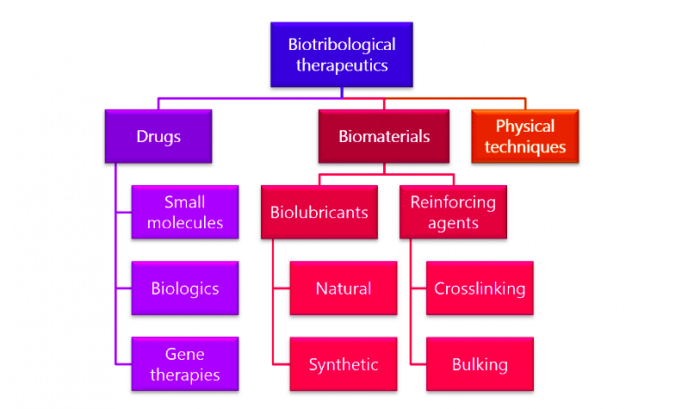
Image credit: B. Cooper
Highlights include:
Drugs. Targeting certain biological pathways with a drug can stimulate the body to return healthy functioning to its biolubrication processes.
- Small molecule drugs. The drugs pilocarpine (Salagen®) and cevimeline (Evoxac®) bind to a receptor which upregulates secretion of saliva to treat dry mouth. Hormone therapies have also been shown useful in increasing mucosal secretions to address vaginal dryness.
- Biologics (“large molecule” drugs). The protein drug interferon α is another treatment which upregulates salivary secretion to treat dry mouth.
- Gene therapies. Delivery of the gene encoding the lubricating glycoprotein known as lubricin has shown preclinical success in protecting cartilage from wear in the treatment of osteoarthritis.
Biomaterials — biolubricants and reinforcing agents. Introducing a lubricating or wear-preventive material to the site of interest can help preserve healthy functioning.
- Naturally-occurring biolubricants. Hyaluronic acid is a polysaccharide naturally found in tear film and synovial fluid, and it is a component of many commercial eyedrops for dry eye and injectable joint lubricants for osteoarthritis. Cellulose derivatives, including carboxymethylcellulose and hydroxypropylmethylcellulose, are found in both eye drops and personal lubricants.
- Synthetically-made biolubricants. Synthetic polymers such as poly(vinyl alcohol) and poly(acrylic acid) are found in some eye drops, Teflon and poly(vinyl pyrrolidone) are incorporated into the surface of implantable repair patches and catheters to prevent friction following surgeries and catheter insertions, and poly(ethylene glycol) and silicone polymers are found in many personal lubricants.
- Crosslinking reinforcement. Polymer crosslinking strategies have shown preclinical success in strengthening osteoarthritic cartilage to increase its wear resistance.
- Bulking reinforcement. Weakening and breakdown of tissue in the urinary sphincter can cause urinary incontinence; this can be treated by injection of polymer gels around the muscle to prevent further weakening.
Physical techniques (non-biological & non-material). This category includes strategies that fall outside the classical designation of drugs or materials, to treat diseases of friction and wear.
- Electrostimulation has been shown in clinical trials to increase salivary secretion to treat dry mouth and thermal conditioning (exposure to moderately high temperatures) has preclinically mitigated high friction following surgery, while ultrasound and laser therapy can be used to treat wear-prone tissues in diseases of chronic wounds and dry skin.
With advances in our understanding of biology and biomechanics, coupled with inventions and refinements in chemical/material synthetic techniques and biomedical/tissue engineering, the future is promising for improved outcomes for patients with diseases of high friction and wear. In particular, due to increased amounts of interdisciplinary science and engineering research, we will begin seeing more multi-pronged approaches to address these biotribological challenges as our bodies continue to function for an increasing number of years without succumbing to wear and tear.
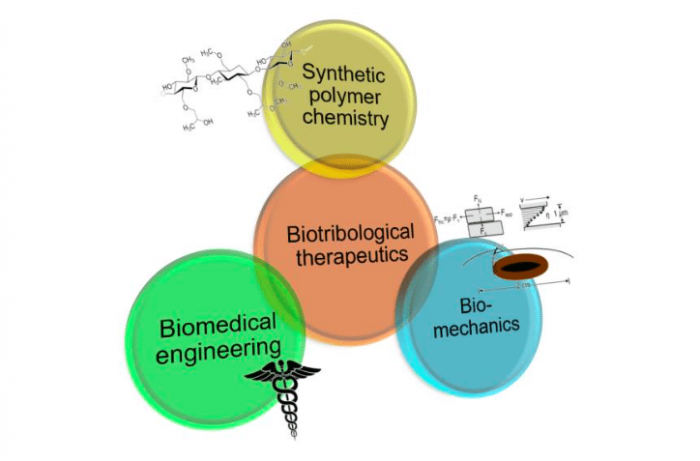
Image credit: B. Cooper
These findings are described in the article entitled Active agents, biomaterials, and technologies to improve biolubrication and strengthen soft tissues, recently published in the journal Biomaterials. The review was written by Benjamin G. Cooper, Catalina Bordeianu, and Mark Grinstaff from Boston University, and Ara Nazarian and Brian D. Snyder from Beth Israel Deaconess Medical Center.









