
Research from the Danish Cancer Society shows that the intake of red and processed meat are the risk factors with the highest impact for the prevention of colorectal cancer in Denmark over the next 30 years. Around 22,000 new colorectal cancer cases could be avoided up to 2045 if Danes totally eliminated processed meat from their diets. Similarly, almost 17,000 new cases could be avoided if Danes totally eliminated red meat from their diets.
This is a bit surprising when comparing the impact of other risk factors for colorectal cancer with the impact of red and processed meat. Obesity, smoking, and alcohol consumption are acknowledged as more serious risk factors for cancer in general, but the impact of these risk factors on the development of colorectal cancer is well overshadowed by the impact of red and processed meat (see attached table).
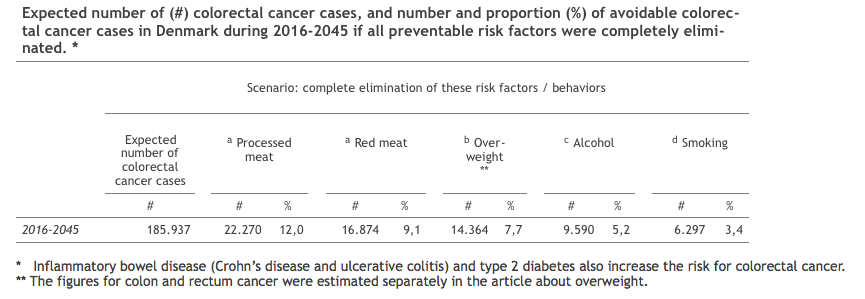
References: a Lourenço et al. (2018). Avoidable colorectal cancer cases in Denmark – The impact of red and processed meat. Cancer Epidemiology 55: 1-7. DOI: https://linkinghub.elsevier.com/retrieve/pii/S1877782118301310; b Andersson et al. (2017). Avoidable cancer cases in the Nordic countries – The impact of overweight and obesity. European Journal of Cancer 79: 106-118. DOI: https://linkinghub.elsevier.com/retrieve/pii/S0959804917308663; c Andersson et al. (2018). Avoidable cancers in the Nordic countries – The impact of alcohol consumption. European Journal of Cancer. DOI: https://linkinghub.elsevier.com/retrieve/pii/S0959804918307767 Andersson et al. (2018). Tackling the tobacco epidemic in the Nordic countries and lower cancer incidence by 1/5 in a 30-year period – The effect of envisaged scenarios changing smoking prevalence. European Journal of Cancer. DOI: https://linkinghub.elsevier.com/retrieve/pii/S0959804918302399. Credit: Danish Cancer Society
We used the Prevent model to calculate these figures. The model uses data on disease incidence (provided by the NORDCAN database); the relative risk estimates for the association between colorectal cancer and intake of red and processed meat (provided by the World Cancer Research Fund); demographic data and its predicted development (provided by Statistics Denmark); and information on red and processed meat intake in Denmark (provided by the Technical University of Denmark – see attached illustration).
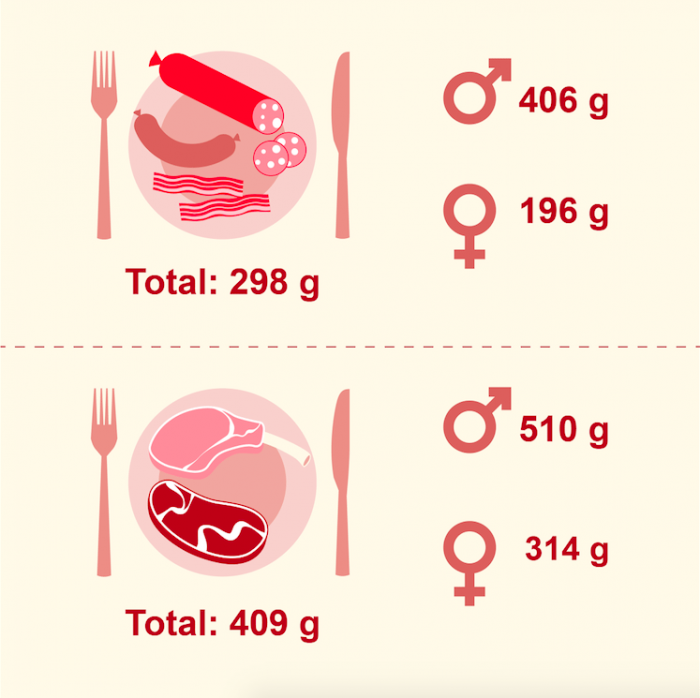
Mean intake of processed and red meat per week in Denmark. Mean intakes calculated from data provided by the report The Dietary Impact of Meat [In Danish: Køds rolle i kosten.] Credit: Danish Cancer Society
A considerable public health impact is theoretically possible.
- If Danes completely stopped eating processed meat, 22,270 cases could be avoided over the next 30 years.
- A modest reduction in the consumption of processed meat (up to 25 gram/day) could result in the avoidance of 12,233 new colorectal cancer cases.
- The correspondent figures for red meat are 16,874 and 5,129 avoidable cases for either total elimination or a modest reduction, respectively.
- The largest impact is observed for men in all scenarios, which is easily explained by the higher intakes of both red and processed meat among Danish men.
These results can be difficult to compare directly with similar estimates from other countries. Other researchers use different models, and the input into the models might vary considerably. However, it is possible these results would be similar in countries with comparable high intakes of red and processed meat.
It should be also noted, that our estimates only work with elimination/reduction scenarios for the consumption of red and processed meat. We did not take into the account the possible effects of meat substitution with other foods. (e.g. increased intake of fish, poultry, pulses, vegetables, whole grains or other foods). The evidence shows that a higher intake of whole grains decreases the risk of colorectal cancer, and even though the evidence is not conclusive about fish, it might also decrease the risk for colorectal cancer. Also, overweight, alcohol consumption and smoking are relevant risk factors in this equation. The real prevention potential for colorectal cancer might be even higher if Danes both reduce their consumption of red and processed meat, increase the consumption of whole grain foods and fish, lose weight and cut down on alcohol and smoking. The prevention potential for colorectal cancer might be even higher, if Danes both reduce their consumption of red and processed meat, and increase the consumption of foods such as whole grains and fish.
The association between a higher risk for colorectal cancer and the intake of meat, with particular emphasis on the intake of processed meat, has been well established previously by both the World Cancer Research Fund International / American Institute for Cancer Research and the International Agency for Research on Cancer. WHO and the European Code Against Cancer are, therefore, straightforward in their recommendation to avoid processed meat and limit the intake of red meat (max 500-gram cooked weight per week).
Changing dietary habits is not an easy thing to ask people to do, and it is only possible if both knowledge of risk factors and their potential impact, as well as structural approaches (e.g. reducing red and processed meat offers in canteens; and retail initiatives, like smaller packages for processed meat products), are in place. A high consumption of processed meat (and to some extent red meat) is not only associated with a higher risk for colorectal cancer but also a higher risk for type 2 diabetes, cardiovascular diseases, preterm and all-cause mortality. Thus, the public health impact of a reduction in red and processed meat consumption is considerable and should be taken into account by both politicians and public health planners alike.
These findings are described in the article entitled Avoidable colorectal cancer cases in Denmark – The impact of red and processed meat, recently published in the journal Cancer Epidemiology.
This work was conducted by Sofia Lourenço, Vibeke Berglund Gunge, Camilla Liv Erthmann Andersen, Anne-Sofie Q. Lund, Brian Køster and Gitte Laub Hansen from the Department of Cancer Prevention and Information at the Danish Cancer Society and Therese M.-L. Andersson from the Karolinska Institutet, Sweden.









