The liver is one of the major organs involved in metabolic function because it performs the important function of converting excess carbohydrates and proteins into fatty acids and triglycerides.
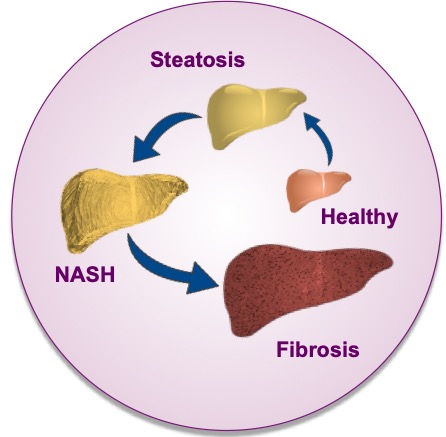
Under normal conditions, these compounds are stored properly and there are no health concerns; however, certain bodily conditions can result in improper accumulation of fat within liver cells. This can lead to inflammation, which in some people, progresses to cirrhosis — a stage of liver disease where permanent damage and scarring occur.
Non-alcoholic fatty liver disease (NAFLD) is an umbrella term used to describe a range of liver conditions affecting individuals with excessive fat storage in their liver cells, even in the absence of significant alcohol consumption. Obesity and insulin resistance are associated with fat accumulation in the liver, and obesity is a significant risk factor for NAFLD [1].
In keeping with the rising rates of obesity, NAFLD prevalence is also increasing. In the United States alone, there are greater than 30 million people diagnosed with NAFLD [2]. Alarmingly, the prevalence of NAFLD is also escalating in children [3]. Not surprisingly, NAFLD is tightly linked to a cluster of metabolic disorders such as increased abdominal fat, high blood pressure, and high blood levels of triglycerides.
To date, there are no effective pharmacological agents that can prevent the development and progression of fibrosis in NAFLD patients. Although the looming presence of liver disease in modern society may seem frightening, there is a lot of research being conducted today to identify better ways to diagnose, treat, and prevent NAFLD, before it has a chance to progress to the point of no return.
DNA Methylation & Why It’s Important
DNA methylation is a molecular process that helps the body to self-repair, fight infection, get rid of environmental toxins, and adapt to environmental stimulation. DNA methylation refers to the mechanism of adding a methyl group (a single carbon atom flanked by three hydrogen molecules) to a nucleotide sequence to change the activity of the DNA without actually changing its sequence. DNA methylation most commonly affects a cytosine-guanine pair (CpG sites), by modifying the cytosine residue. When this happens in the promoter region of a gene, the effect is typically a repression of gene expression.
Credit: Johanna K. DiStefano
Under normal conditions, CpG sites typically remain unmethylated, thereby allowing for unrestricted gene expression. However, higher or lower levels of DNA methylation can affect cellular homeostasis and are becoming increasingly associated with a variety of human diseases. Faulty methylation can result from physiological effects brought on by such things as an unhealthy diet, high levels of prolonged stress, and sometimes even cancer.
In our recent paper “Differentially methylated loci in NAFLD cirrhosis are associated with key signaling pathways”, published in Clinical Epigenetics, we compared patterns of DNA methylation in biopsy-proven cirrhotic livers with normal livers obtained from obese Caucasian female NAFLD patients, with no history of significant alcohol or drug abuse and matched by age, sex, body mass index and type 2 diabetes [4].
We identified more than 4000 CpG sites showing differential methylation between the two groups. When we looked at the clustering of these CpG sites, we identified approximately 200 areas of concentrated methylation-a phenomenon known as CpG islands (CGIs). The top signaling pathways found for these CGIs were found to be related to the production of nitric oxide and reactive oxygen species (ROS).
Nitric oxide is a widespread signaling molecule involved in biological functions such as regulating blood flow by increasing blood vessel dilation. Nitric oxide has a particularly important role in liver biology: under normal stress stimuli, production of this molecule helps to protect against hepatic injury. However, prolonged injury leads to generation of increased levels of nitric oxide, resulting in the production of reactive nitrogen species that target and damage DNA, lipids, and proteins in a similar fashion as ROS [5]. The ROS pathway is important because it can serve as a signaling molecule by cells as a part of their protective response against harmful bacteria. However, when there is an imbalance of ROS production oxidative stress can occur and have harmful effects on the cell.
Although ROS appear to have roles in lipotoxicity — a physiological condition that can lead to cellular dysfunction and cell death — and inflammation, the efficacy of antioxidant treatments in NAFLD patients was poor. In the future, targeting these two pathways could serve as a potential therapeutic approach for NAFLD-related liver diseases.
In addition to our work, four other studies have investigated liver-specific methylation profiles in NAFLD patients [6-9]. Despite different study designs, study sample composition, and analytical strategies, we identified 86 common differentially methylated CpG sites across at least three of the five reports. In all five studies, however, only four genes showing differential patterns of CpG methylation were observed. These genes include 1) aquaporin 1 (AQP1), which encodes a water channel that is overexpressed in fibrosis and cirrhosis, and appears to promote hepatic fibrosis through mechanisms involving the pathological development of new blood vessels [10]; 2) fibroblast growth factor receptor 2 (FGFR2), which when stimulated with its ligand fibroblast growth factor (FGF), initiates a signaling response within cells.
FGF2 levels have been shown to increase in conjunction with hepatic stellate cell activation [11] and liver cirrhosis [12], while knockdown of FGF2 expression in the carbon tetrachloride mouse model of hepatic injury was associated with decreased collagen expression and protection from liver fibrosis [13].
Hepatic stellate cells are the main fat-storing liver cell that works to help maintain a cells’ normal cellular membrane structure in an inactivated state, however, when it undergoes activation to a myofibroblast it increases the production of proteins that in turn increase the thickness of its extracellular matrix-promoting fibrosis. The fourth gene, retinol-binding protein 5 (RBP5), functions to transport retinol, which is stored primarily in the liver, while the remaining gene, O6-methylguanine-DNA-methyltransferase (MGMT), has a yet-unexplored role in NAFLD-related liver disease. In all cases, each gene was hypomethylated, suggesting that transcription levels were higher in NAFLD fibrosis. This is consistent with what we would expect, based on our knowledge of the function of the corresponding proteins.
What Does It All Mean & What’s Next?
The findings indicate these four genes could represent targets for the development of new therapeutics in the treatment of NAFLD-related fibrosis. Important next steps for this work are to confirm the methylation patterns of these genes in a cohort of ethnically diverse patients spanning the histological spectrum of NAFLD. Future studies focused on teasing out the biological consequences of these altered methylation states in NAFLD development and progression will also be important.
Finally, determining the extent to which DNA methylation patterns in the liver are represented in other metabolically relevant tissues will be critical for the development of non-invasive biomarkers for to detect disease as early as possible and treat it properly before it progresses to a more damaging and irreversible state.
These findings are described in the article entitled Differentially methylated loci in NAFLD cirrhosis are associated with key signaling pathways, recently published in the journal Clinical Epigenetics. This work was conducted by Glenn S. Gerhard from Temple University School of Medicine, Ivana Malenica, Lorida Llaci, and Johanna K. DiStefano from the Translational Genomics Research Institute, and Xin Chu, Anthony T. Patrick, and Christopher D. Still from the Geisinger Obesity Institute.
References:
- Fabbrini, E., S. Sullivan, and S. Klein, Obesity and nonalcoholic fatty liver disease: biochemical, metabolic, and clinical implications. Hepatology, 2010. 51(2): p. 679-89.
- Lazo, M., et al., Prevalence of nonalcoholic fatty liver disease in the United States: the Third National Health and Nutrition Examination Survey, 1988-1994. Am J Epidemiol, 2013. 178(1): p. 38-45.
- Dart, A.B., et al., Earlier onset of complications in youth with type 2 diabetes. Diabetes Care, 2014. 37(2): p. 436-43.
- Gerhard, G.S., et al., Differentially methylated loci in NAFLD cirrhosis are associated with key signaling pathways. Clin Epigenetics, 2018. 10(1): p. 93.
- Iwakiri, Y. and M.Y. Kim, Nitric oxide in liver diseases. Trends Pharmacol Sci, 2015. 36(8): p. 524-36.
- Ahrens, M., et al., DNA methylation analysis in nonalcoholic fatty liver disease suggests distinct disease-specific and remodeling signatures after bariatric surgery. Cell Metab, 2013. 18(2): p. 296-302.
- de Mello, V.D., et al., Human liver epigenetic alterations in non-alcoholic steatohepatitis are related to insulin action. Epigenetics, 2017. 12(4): p. 287-295.
- Hotta, K., et al., Identification of the genomic region under epigenetic regulation during non-alcoholic fatty liver disease progression. Hepatol Res, 2017.
- Murphy, S.K., et al., Relationship between methylome and transcriptome in patients with nonalcoholic fatty liver disease. Gastroenterology, 2013. 145(5): p. 1076-87.
- Huebert, R.C., et al., Aquaporin-1 facilitates angiogenic invasion in the pathological neovasculature that accompanies cirrhosis. Hepatology, 2010. 52(1): p. 238-48.
- Fibbi, G., et al., Functions of the fibrinolytic system in human Ito cells and its control by basic fibroblast and platelet-derived growth factor. Hepatology, 1999. 29(3): p. 868-78.
- Jin-no, K., et al., Plasma level of basic fibroblast growth factor increases with progression of chronic liver disease. J Gastroenterol, 1997. 32(1): p. 119-21.
- Yu, C., et al., Role of fibroblast growth factor type 1 and 2 in carbon tetrachloride-induced hepatic injury and fibrogenesis. Am J Pathol, 2003. 163(4): p. 1653-62.









