
HIV was first thought to have entered the United States in the 1970s. Initially, it primarily affected drug users and gay men. This affiliation, along with the increased occurrence of HIV, created a great stigma against people with HIV and especially against those of the LGBT community, bolstering things like homophobia. HIV did not stay within just populations of drug users and gay men. It was a highly virulent disease that spread across the world, creating a global pandemic.
Initially, it was a death sentence to acquire HIV, which would eventually become AIDs, because there was little we could do to treat it. As scientists continued to work on ways to treat and cure it, we developed more and better antiretroviral therapy (ART) drugs that extended the life of those with HIV to the point where they can not live a complete life.
Recently, the Center for Disease Control and Prevention (CDC) announced that the sexual transmission of HIV cannot occur when individuals have undetectable viral loads. Being undetectable means having such a low amount of HIV that they cannot move from the host to another person via sexual intercourse. Having these low levels of HIV means that you cannot infect another person as well as mitigating many of the problems associated with having HIV. The CDC arrived at its conclusion after assessing the results of three different studies done concerning this matter. The studies looked at thousands of couples and thousands of sexual acts that were done without pre-exposure prophylaxis (PReP) or condoms. They found that those with undetectable levels of HIV did not give the virus to HIV-negative partners.
ART
Antiviral drugs are simply drugs that are used to treat viral infections and they belong to a large class of drugs called antimicrobials, which also includes antibiotics, antifungals, and antiparasitics. Nowadays, most of them are harmless to the host as they have high enough specificity and low side effects to not hurt the person taking them. For individuals with HIV, they are usually taking antiretroviral therapy, which is varying cocktail of different antiviral drugs. Individuals take multiple drugs rather than just one because they prove to be far more effective than a single one. Since there is no known cure for HIV, the purpose of ART is to slow down the growth rate of HIV to the point that it becomes undetectable.
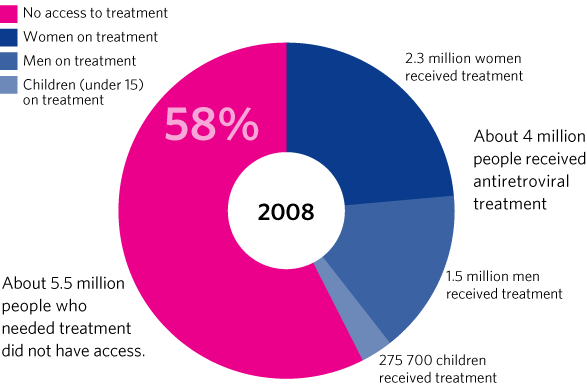
Percentage of people who have access to antiviral treatments. Image from WHO
The ART drugs are inhibitors of HIV functions, which includes its ability to turn its RNA to DNA, to integrate into the host DNA, and to generally infect more cells. These allow the immune system of the infected person to recover and prevents, or at least slows, the HIV from becoming AIDs. The two most known ART are PREP and PEP.
PREP
PReP is a precautionary ART that is taken by those who are at risk of acquiring HIV. It is a combination of two antiviral drugs, tenofovir, and emtricitabine. Tenofovir, used to treat hepatitis B as well, and emtricitabine are inhibitors that prevent the virus from replicating itself. In a time when HIV is a problem from the entire world, the World Health Organization has added tenofovir to its list of essential drugs that would benefit global human health. The CDC found that PReP is capable of reducing the risk of acquiring HIV by 90% through sex and 70% through drug use.
One of the important things to understand about PReP is that it is a commitment. To be highly effective, it must be taken every day. If someone takes it inconsistently they are raising their risk of acquiring an HIV infection. It has been found to be safe for daily use with minimal side effects. To ensure that it becomes highly effective, you must begin taking it at least seven days prior to sex and 20 days prior to things like drug use. It takes a little bit of time for the drugs to be ready to face any HIV occurrences. PReP is not recommended for individuals with HIV because it will not be effective. It is mainly to prevent rather the infection.
PEP
Post-exposure prophylaxis (PEP) is the ART that is taken after you may have been exposed to HIV. It is meant to be taken within 72 hours of potential exposure. It is composed of a few different antiviral drugs that vary from place to place as there are a few effective drugs used in PEP treatments. They are generally around three different drugs. Unlike PReP, which is a long-term commitment, you only have to take PEP for about 28 days to ensure that you do not become infected with HIV. As with most things, PEP is not 100% effective because there may be strains of HIV the cocktail does not cover, which would require some changes to your PEP. There may also be difficulty in taking the PEP for the duration of the treatment. One of the ways that PEP can be ineffective is if someone does not follow their treatment plan.
Problems and The Future
PEP and PReP, among the many other ART, helped to revolutionize how we approach treatment for HIV because they have allowed infected individuals to live a full life. They are not without their problems as they are treatments, not cures. There is much research into curing HIV, which is difficult because HIV is very mutative. There is also the stigma and misunderstanding surrounding HIV and individuals with HIV that we need to address to bring in more support for treatment options.
Additionally, there are places in the world that do not have access to the full range of ART available. One such region is Africa, which is facing a worse HIV epidemic than anywhere else. To address this, we need to be able to reduce the cost of treatment options, increase their effectiveness, and find a cure. Hopefully, this becomes possible within our lifetimes so we can spare future generations this burden.









